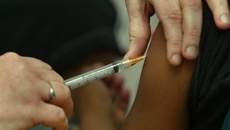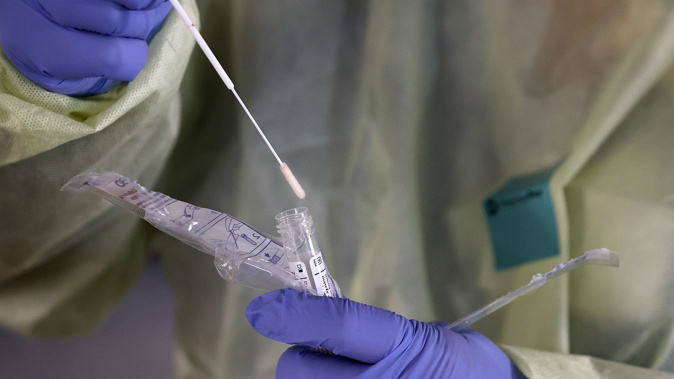
The Government has been urged to keep ramping up capacity for testing, which offers one of New Zealand's best chances of getting on top of the contagion while it still can.
Up to the middle of the month, about 500 tests had been done; yesterday, 1200 tests were carried out, compared with 1500 on Friday and 1000 on Thursday.
There has been also sharp increase in the number of positive cases in New Zealand over recent days, jumping from just a dozen early last week to 66 today.
Dr James Hadfield, a Wanaka-based phylogeneticist with Seattle's Bedford Lab, said that sharp rise shouldn't necessarily be seen as a bad thing.
He said 6000 tests worked out at roughly 1250 per million of New Zealand's population; testing in the United States, which has seen a surge to nearly 23,000 cases earlier in the month, had been running around 75 tests per million population.
Source / James Hadfield
"South Korea, while hard to compare directly with us, has run about 5000 tests per million of population."
Hadfield said the outbreak in Washington state, with more than 1500 cases and more than 83 deaths, had highlighted why quickly getting a greater handle on the number of potential cases was so important.
"What we saw from the experience of Washington state was that, only once we started testing more widely did we start to detect community spread, which is now very challenging to control."
With a better testing regime, scientists were able to use genomics to determine whether positive tests had come as a result of transmissions in the community, or from new cases introduced from overseas.
"So without testing with quite a relaxed case definition and sequencing the positive cases, we were blinding ourselves to the extent of community transmission in Washington."
Hadfield said volume was also critical.
"The more people we are able to test in New Zealand the more positives we'll find, but the percentage of positive tests we get back should drop. If we compare ourselves now with where other countries are, and given how recently we had our first case, we're in a strong position."
Otago University epidemiologist Professor Michael Baker said New Zealand was "almost certain" to have community transmission of Covid-19.
"The good news is that we haven't yet heard of people turning up in hospital with pneumonia and going into intensive care – so that is quite positive."
Baker was aware of one Italian town, Vo, which tested its entire population of 3000, flushed out and isolated around 100 cases, and then stamped out Covid-19 in two weeks.
But he felt such an undertaking in New Zealand would be a "terrible waste of resources".
"This isn't like hepatitis C, where you can make a case for testing everyone. In this case, we could prioritise people with some risk factors, but the key thing is capturing those people who met the criteria.
Less than two months after the first cases began popping up outside China, the basic formula for containing Covid-19 was now "extremely well known" to epidemiologists, he said.
"What has transformed our thinking is that China was able to stop this thing in full flight.
Other countries that have systems quite like our own – such as Taiwan and Singapore – have managed well, too.
"So that makes me hugely optimistic that New Zealand can do the same. We just have to ramp up our capabilities faster. Time is of the essence, and people have got to get tested, diagnosed and isolated very quickly for this to work."
Baker noted that New Zealand didn't have impressive manpower of China, which was able to deploy more than 1800 separate teams of close contact tracers in the outbreak's ground zero of Wuhan.
He has also called for a nationwide lockdown lasting possibly four weeks, which would fire a "pulse" to slow Covid-19's spread.
"The real prize for New Zealand here is being able to come out the other end of this in a post-containment period, where we have eradicated the virus, and are mopping up the occasional case.
"The alternative is that we are forced to go into what's called a suppression mode – which we are now seeing in London, Berlin, and all across Europe – where they know the health system can't cope, so are brutally lowering rates.
"That's a very tough state to be in because the only exit strategy is a vaccine or anti-viral – and that could take a year to 18 months. We want to be more like Singapore and Taiwan, and much less like Europe."
The Ministry of Health's Director-General of Health, Dr Ashley Bloomfield, has said testing in New Zealand has increased in line with the number of people who officials felt needed it, based on links to travel.
Asked why many people were still being declined testing, Bloomfield said patients needed to meet the case definition – which was that they should have a history of overseas travel, or a close contact with a confirmed, probably or suspected case, and have symptoms.
"So we shouldn't be at this point – and we can't be – testing everyone who has symptoms of an upper or lower respiratory tract infection," he said.
"It's important that we test the right people, and not people who are at low risk."
More testing kits have been sourced from Singapore to ensure New Zealand had enough capacity and community-based assessment centres – including drive-through hubs in Auckland - were being rolled out around the country.
Bloomfield said it was important lab workers were getting rest amid the heavy demand but added this wouldn't impact on testing capacity.
"I'm hoping and expecting they will be giving staff down-time but we are not expecting delays in testing results."
Take your Radio, Podcasts and Music with you